Chronic Inflammation? Here’s How Altering Your Lifestyle Can Help
A wide array of diseases have been linked with chronic inflammation. Follow an anti-inflammatory lifestyle to reduce your risks.
Your immune system is like a home security system. When you suffer an injury or infection, it sets off an alarm—what we know as an inflammatory response—by sending immune cells to neutralize viruses, bacteria, and other intruders that breach your outer defenses, thereby protecting healthy cells and tissues from damage. Essentially, inflammation is part of the healing process, and without it, our injuries and illnesses would never heal. That’s the good part. The bad occurs when you experience chronic inflammation.
Chronic inflammation can persist for months or years. In such instances, the immune system engages in a prolonged “friendly fire” of sorts, damaging cells and tissues throughout the body over time.
ANTI-INFLAMMATORY FOODS
One easy way to reduce inflammation in your body is through your diet. You’ll find specifics in our post “Anti-Inflammatory Foods: Can They Reduce Chronic Inflammation?”
The chronic inflammation process has been linked to a broad array of diseases, some of them life-threatening. While inflammation from an acute injury may manifest as pain, swelling, redness, and other symptoms, chronic inflammation can go unnoticed and unchecked for years.
Fortunately, you can reduce inflammation in your body by eating a healthful diet, getting regular exercise and adequate sleep, and finding ways to minimize or conquer stress in your life. Following an anti-inflammatory lifestyle can help you feel better and, in some cases, may reduce your risk of chronic disease.
What Is a Chronic Inflammatory Condition?
Chronic inflammation may arise if the source of acute inflammation is not removed from the body, or if you experience prolonged exposure to chemicals or other inflammatory agents.
Oftentimes, chronic inflammation is the byproduct of an autoimmune disorder, which occurs when the immune system mistakenly attacks healthy tissues. As such, inflammation is a common factor in many diseases, such as:
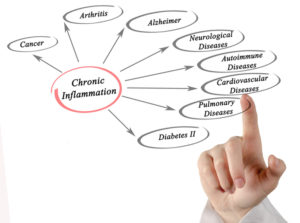
Cancer, arthritis, and Alzheimer’s disease are among the many afflictions that can be indicative of chronic inflammation. [Photo: © Vaeenma | Dreamstime ]
- Digestive diseases: A wayward immune response produces inflammation that damages the intestinal lining (causing Crohn’s disease) and the colon (resulting in ulcerative colitis). An abnormal immune sensitivity to gluten (a protein in wheat, rye, and barley) triggers inflammation that causes celiac disease. (See also Gluten Free & More‘s post on how to reduce inflammation.) And, in the mouth, where the digestive system begins, inflammation from periodontal disease can wreak havoc on your gums.
- Respiratory diseases: Asthma is characterized by chronic inflammation of the bronchial tubes, while prolonged inflammation in the sinuses leads to the pain of chronic sinusitis. An abnormal immune response also is to blame for seasonal allergies, such as hay fever.
- Diabetes: Type 1 diabetes is an autoimmune disorder that damages insulin-producing cells in the pancreas. In one study, researchers identified chronic inflammation of the digestive tract and unique changes in gut bacteria in people with type 1 diabetes (Journal of Clinical Endocrinology & Metabolism, January 2017). “Our findings indicate the individuals with type 1 diabetes have an inflammatory signature and microbiome that differ from what we see in people who do not have diabetes or even in those with other autoimmune conditions, such as celiac disease,” the study’s senior author, Lorenzo Piemonti, MD, of San Raffaele Hospital in Milan, Italy, said in a statement. Studies also have found higher levels of inflammation in people with type 2 diabetes, the most common form of diabetes.
- Skin disorders: Inflammation is at the root of several skin diseases, including psoriasis, eczema, and rosacea.
- Joint diseases: Chronic inflammation, pain, and joint damage characterize rheumatoid arthritis as well as ankylosing spondylitis, a type of inflammatory arthritis that affects primarily the spinal joints. Inflammation caused by uric acid deposits in the joints leads to painful gout flare-ups. And, inflammation from another autoimmune disorder, systemic lupus erythematosus (lupus), can harm the joints, as well as the heart, lungs, blood vessels, kidneys, skin, and brain.
Other research suggests that inflammation can have deleterious effects on the brain and might play a role in Alzheimer’s disease. Furthermore, high levels of inflammation are common in people with depression, suggesting a role of chronic inflammation in the development of depressive disorders.
How Inflammation Relates to Cardiac and Cancer Concerns
Several investigations have found that chronic inflammation plays a role in atherosclerosis, or “hardening” of the arteries, and that people with elevated levels of inflammatory markers are at increased risk of cardiovascular events, such as heart attack and stroke.
Experts believe your immune system perceives fatty, cholesterol-laden plaques lining your artery walls as abnormal, and it sends white blood cells to shield them from your bloodstream. However, this inflammatory response can make the plaques vulnerable to rupture, spilling their contents out into the bloodstream and exposing parts of the vessel wall not normally in contact with blood. This process can trigger platelet activation and formation of blood clots that may cause heart attacks or ischemic strokes.
Chronic inflammation also may factor into DNA damage and gene alterations associated with several types of cancer. For example, having inflammatory bowel disease (ulcerative colitis and Crohn’s disease) significantly increases the risk of colorectal cancer; chronic inflammation of the liver (hepatitis) increases the risk of liver cancer; and inflammation of the esophagus (Barrett’s esophagus) is a known risk factor for esophageal cancer.
Additionally, researchers have found pockets of inflammation in cancerous prostate cells. Research into inflammation’s role in cancer continues.
What Could Cause Inflammation in Your Body?
Several modifiable factors are known to promote chronic inflammation. By avoiding or optimizing these risk factors, you might minimize the damaging effects of chronic inflammation:
- A poor diet: What you eat may contribute to inflammation. Avoid pro-inflammatory foods, such as high-fat red meats, full-fat dairy products, fried foods, processed foods, and added sugars. Instead, consume plenty of antioxidant-rich fruits and vegetables (good examples include beans, broccoli, leafy greens, blueberries, oranges, and strawberries) that have anti-inflammatory properties. Replace unhealthy saturated and trans fats with healthier fats: Use olive oil instead of butter, and consume anti-inflammatory omega-3 fatty acids (found in salmon, mackerel, tuna, and other cold-water fish).
- Lack of exercise: People who lead sedentary lifestyles tend to have higher levels of inflammation. But, increasing your physical activity can reduce inflammation. In fact, in one study, researchers reported that people who regularly adhered to guidelines recommending at least 2½ hours of moderate-to-vigorous physical activity a week had significantly lower levels of two inflammatory markers—C-reactive protein and interleukin 6—over a 10-year period as compared to those who did not adhere to the guidelines (Circulation, Aug. 21, 2012).
- Obesity: Fat cells aren’t just inactive storage centers, but rather tiny factories that produce inflammatory chemicals called cytokines. The inflammation resulting from an overabundance of fat cells may explain, in part, obesity’s connection to several chronic diseases, including cardiovascular disease, type 2 diabetes, and certain cancers. If you’re overweight or obese, work with your healthcare team to lose weight via a healthy diet, exercise, and, if necessary, medical weight loss therapy.
- Smoking: Cigarette smoking and exposure to secondhand smoke can increase inflammation. If you smoke, ask your physician about nicotine replacement therapy, medications, counseling, and other strategies to help you kick the habit.
- Emotional stress: Anxiety and stress are well known risk factors for chronic inflammation. In one study, researchers reported that stress can inhibit the body’s ability to use the hormone cortisol to manage inflammation (Proceedings of the National Academy of Sciences, April 2, 2012). “Inflammation is partly regulated by the hormone cortisol, and when cortisol is not allowed to serve this function, inflammation can get out of control,” study author Sheldon Cohen, PhD, of Carnegie Mellon University, said in a statement. Tell your doctor if you chronically feel anxious, and work on ways to manage the stress in your life. Consider stress-relieving techniques such as mindfulness meditation, or simply find a hobby you enjoy that can take your mind off your worries.
- Sleep disorders: Sleep problems, such as obstructive sleep apnea, have been linked with increased inflammation. Tell your doctor about any signs of sleep apnea, such as excessive daytime sleepiness, loud snoring, or interruptions in breathing during sleep (as reported by your bed partner).
Originally published in 2017, this post is regularly updated.


 Vestibular Migraine Diet
Vestibular Migraine Diet  Bone Spurs on the Spine
Bone Spurs on the Spine  Knee Injections for Osteoarthritis Pain Relief
Knee Injections for Osteoarthritis Pain Relief 
Chronic inflammation is behind myriad conditions that plague us. What causes it? Lack of exercise, a poor diet, obesity, smoking, stress, and sleep disorders all can contribute.
© One Photo | Dreamstime