Mild Heart Attack Symptoms and What to Do When It Happens
Mild heart attack symptoms can mimic those of a more serious heart attack. You can't tell the difference by symptoms alone. All heart attack symptoms are major.
What is a “mild heart attack”? You may have heard the expression and wondered exactly what it means. A bone can have a hairline fracture or a major break. A stroke can have relatively minor consequences or be severely debilitating. So can a heart attack be mild or major?
The short answer is yes. What determines whether a heart attack is minor or major is the extent of damage to the heart muscle itself.
Keep in mind, however, that mild heart attack symptoms can resemble those of a more serious heart attack. That’s because heart attack causes refer to the blockage in one or more coronary arteries, no matter what kind of lasting consequences they leave behind. Heart attack is either complete blockage of a coronary artery, called ST-elevation myocardial infarction (STEMI), or partial blockage called non-ST elevation MI (NSTEMI). A person cannot tell the difference by symptoms, and the treatment is different: STEMI is treated with a stent, and NSTEMI treatment starts with anticoagulation and stent as a second line treatment.
But whether they’re mild, major, or somewhere in between, heart attack symptoms should be treated with emergency care.
NEW HYPERTENSION GUIDELINES
Does 140/90 still serve as the threshold for high blood pressure? New hypertension guidelines issued by the American College of Cardiology (ACC) and American Heart Association (AHA) call for a lower reading. Click here for our report.
What Causes a Heart Attack?
By definition, a heart attack is the result of blockage in an artery that supplies blood to the heart muscle. These blood vessels are called coronary arteries. You’ve probably heard the term “coronary artery disease,” or CAD. That just means that there’s plaque buildup in one or more of the heart’s arteries, and that it’s reducing or blocking blood flow in those arteries. The plaque is a waxy substance that includes LDL cholesterol, fats, and other waste products from your bloodstream.
The process of plaque building up in your arteries is called atherosclerosis. You may know it by a more familiar name: “hardening of the arteries.” This buildup takes place over many years.
There are some less-common heart attack causes, too. One of your coronary arteries could spasm and shut off blood flow to the heart muscle. Sometimes smoking or illicit drugs can result in coronary artery spasm. A spasm can occur in a coronary artery that isn’t affected by atherosclerosis.
Also unusual, but still possible, is a tear in the inner wall of a coronary artery; this is called a spontaneous coronary artery dissection. An artery has three walls or layers. When blood seeps through a tear in the inner layer, it can become trapped and bulge inward. As a result, blood flow through that artery becomes blocked.
Heart Attack Symptoms
The clinical name for a heart attack is a myocardial infarction. If one is in your future, of course you want it to be a mild heart attack. Symptoms for any type of heart attack, however, include the following signs:
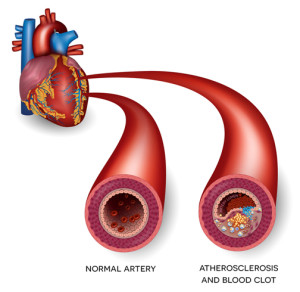
Pictured: a normal artery and (at right) one showing a blood clot. (Photo: © Guniita | Dreamstime.com)
- Chest pain, in many cases pain that comes and goes. It may be centered in the chest or spread from one side to the other.
- Shortness of breath.
- Nausea, sometimes with vomiting.
- Pain or tingling in one or both arms. Don’t be lulled into a false sense of security if the pain is only in your right arm. Arm discomfort due to a heart attack isn’t limited to the left side.
- Jaw pain, neck pain, or back pain.
- Breaking into a cold sweat.
- Feeling unusually tired, sometimes for days.
Symptoms may last for a few minutes and then subside, only to return again. Symptoms that come and go should be taken seriously as clues that you may be having a heart attack. Many heart attack survivors describe chest discomfort as “pressure,” rather than “pain.” Don’t be thrown off if you don’t feel a sudden, sharp pain in the middle of your chest. It may feel as though something is squeezing your heart or that something is pressing on your chest.
Understand, too, that major or mild heart attack symptoms vary from person to person. So if the pain or pressure you’re feeling in your chest seems minor, don’t dismiss it as unimportant.
One study found that patients with mild heart attack symptoms (pain or discomfort that starts slowly and gradually worsens) take about eight hours to seek care, while those with sudden heart attack symptoms take less than three hours to seek care. The American Heart Association recommends receiving treatment within two hours to reduce death, regardless of symptoms.
People who have a greater tolerance for pain tend to ignore heart attack signs that feel tolerable. Don’t try to tough it out or worry that you’re inconveniencing people around you by revealing your symptoms.
You should also keep in mind that if you have already had one heart attack, the signs of a second event may be much different.
Anxiety as a Heart Attack Symptom
One other common heart attack symptom is anxiety, or a vague but undeniable feeling that something’s wrong.
Research shows that a heart attack causes victims to feel like they’re having a panic attack. But this is a dangerous assumption. Rather than get help immediately, some individuals having a heart attack want to chalk up their symptoms to indigestion or anxiety or feeling worn out from too much exertion.
In addition, if the pressure in your chest isn’t too uncomfortable and you’re just a little short of breath, you may think you’re having some mild heart attack symptoms. This could lead you to not take them seriously.
(Note: There can be gender differences that reveal heart trouble; there heart attack symptoms common in men, and heart attack symptoms common in women.) see our posts “Heart Attack Symptoms in Men: 5 Common Signs” and “Heart Attack Symptoms in Women.”)
What Is a Silent Heart Attack?
It’s true that some people have what are sometimes referred to as silent heart attacks. These result from temporary blockages in the coronary arteries. Sometimes they don’t even produce mild heart attack symptoms, but many times they do. Evidence of a silent heart attack may only appear much later when your doctor is examining your heart for other reasons.
Silent heart attacks usually cause the same symptoms as other heart attacks but they are milder and don’t last as long. Because they may never result in a visit to the ER, they remain silent.
But you can’t count on a heart attack to be temporary or to cause only minimal damage. So treat major or minor heart attack symptoms as an emergency. The faster you seek medical help for a heart attack, the less damage your heart will suffer. A disruption of blood flow to the heart is a problem, and there will be consequences.
If you have risk factors for a heart attack, including high LDL cholesterol, high blood pressure, smoking, obesity, diabetes, or a family history of heart disease, and you start to feel heart attack symptoms of any kind, call 911. Don’t try to drive yourself to a hospital. Your symptoms may become overwhelming, placing yourself and other motorists at risk on the road.
Make sure your loved ones know the symptoms of a heart attack and what to do if you or someone in your home starts to experience one. Sometimes fast treatment is what makes the difference between a heart attack being mild or major.
Originally published in 2016, this post is regularly updated.
SOURCES


 News Briefs February 2024
News Briefs February 2024  Savor the Sweet Potato
Savor the Sweet Potato  What Are the Dangers of Erythritol?
What Are the Dangers of Erythritol? 
© Kts | Dreamstime.com