Bone Pain? Consider These Imaging and Screening Options
When it comes to stiff, sore bones and joints that won’t stop aching, the medical community has a significant array of test and technologies available to get at the root of the bone pain.
If you’ve been feeling bone pain, your doctor may take one look at that stiff, swollen joint or that loss of motion and suspect that what you’ve got is the inevitable onset of age-related osteoarthritis (OA) or the autoimmune disorder that leads to rheumatoid arthritis (RA).
But to refine that diagnosis, he or she will turn to science and technology to get at the root of your bone pain—and the heart of your treatment. It will probably start with imaging, and may even require a bone density test.
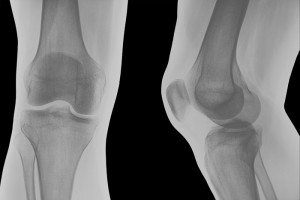
X-Rays
X-rays remain the most important imaging method for determining the severity of your arthritis or the cause of bone pain. Though x-rays show only the position of the bones, the space between bones is an accurate reflection of how much healthy cartilage remains. Narrowing of this space over time is associated with loss of cartilage and can be used to monitor the further advance of osteoarthritis and rheumatoid arthritis.
OA and RA look quite different on x-rays. With RA, small erosions or destruction of the bone can be seen, as can thinning of the bones around the joints (periarticular osteopenia). With OA, you will see tiny irregular outgrowths or bone spurs (osteophytes).
MRI/Magnetic Resonance Imaging
Since X-ray evidence for rheumatoid arthritis may not be apparent until you have the disease for six to 12 months or longer, physicians are turning to magnetic resonance imaging (MRI) to help with earlier detection. Some evidence suggests that MRI may detect inflammation in joints without any apparent clinical inflammation in patients with early RA.
Ultrasound
Due to its low cost, absence of radiation, and speed of imaging, ultrasonography is an attractive method of imaging. Compared to standard X-rays, ultrasound may be more effective at detecting early-stage bone erosion.
Laboratory Tests for Bone Pain Diagnosis
Though there are no current blood tests to confirm the presence of osteoarthritis, several lab tests are being investigated. Researchers are studying certain blood biomarkers, micro RNAs, that may predict which patients will develop OA that necessitates joint-replacement surgery.
For RA, a complete blood count measures the amount of red blood cells, white blood cells, and platelets in your blood, as well as other key blood levels.
- An elevated white blood cell count may suggest inflammation due to RA.
- A low red blood cell count (low hematocrit) often indicates an iron deficiency or an anemia of chronic disease. Since 50 percent of people with RA have such anemia, it adds to circumstantial evidence for RA.
- A blood chemistry screen also may help identify damage to other organs, such as the kidneys, that may be affected by RA.
- It is important to get baseline liver function tests prior to starting RA medications. Liver enzymes can also be elevated in chronic hepatitis B or C, which can cause an inflammatory arthritis similar to RA.
Your doctor also may call for lab tests that look for signs in the joint fluid. If fluid has accumulated in a joint, your doctor may remove some with a needle in a procedure called aspiration. The fluid can be tested for signs of increased inflammation that would be seen with RA, or it can detect any evidence of infection. Analysis of the fluid can also help rule out gout, a form of inflammatory arthritis.
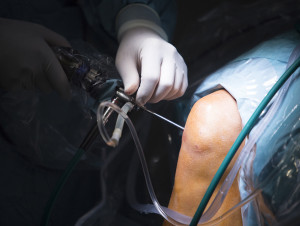
Arthroscopy
This is a minimally invasive surgical procedure in which a doctor looks for joint damage by using an arthroscope, a small camera inserted through a 1-centimeter incision into the joint space.
Used most frequently on the knee, the procedure lets a doctor examine the internal structures and check for damage to ligaments, cartilage, or menisci that may be treated arthroscopically.
Complications Beyond the Joints
- Arthritis and cardiovascular assessment: Research has shown that people with rheumatoid arthritis are at increased risk for cardiovascular disease. In fact, evidence suggests that the cardiovascular risk posed by RA is comparable to that of a leading cardiovascular disease risk factor, diabetes.
- An osteoarthritis-cardiovascular connection? While RA is a well-established cardiovascular risk factor, the effects of OA on heart health are not well understood. One study found that people with OA——especially those with severe OA requiring joint replacement—were at greater risk of cardiovascular problems. Another found that people with symptomatic hand OA faced increased cardiovascular risks.
- Reducing cardiovascular risks: After diagnosing RA, your doctor should screen for cardiovascular risk factors—such as high blood pressure, abnormal cholesterol levels, diabetes, obesity, and smoking—and work with you to manage them and reduce your risk.
- Rheumatoid arthritis and extra-articular manifestations: In addition to its damaging effects on the joints and the cardiovascular system, RA may affect a number of other areas of the body. RA may cause painful breathing, shortness of breath, scarring of the lungs, and lung nodules. In some cases, RA-related lung problems can develop before joint symptoms. Additionally, the incidence of chronic obstructive pulmonary disease (COPD) in people with RA is double that of those without the disease.
People with RA also should be aware of potential kidney disorders and gastrointestinal (GI) problems. Evidence suggests that RA patients may be more likely to develop GI disorders such as stomach ulcers, bleeding, infectious colitis, and diverticulitis.
RA can manifest in the skin as nodules or rashes, and it can cause peripheral neuropathy, nerve damage characterized by numbness, tingling, or burning pain. It commonly causes poor sleep and fatigue. The pain and difficulties associated with the disease also can lead to depression and anxiety.
Another common consequence of RA is osteoporosis, a loss of bone mass that increases your risk of fractures. Compounding the problem is that RA patients (and arthritis patients in general) are at a greater risk of falls and fall-related injuries.
Some patients with RA develop ocular (eye) complications, such as dry eye, inflammation of the blood vessels in the white of the eye (scleritis), and inflammation of the iris (iritis, or anterior uveitis). If you have RA and no eye symptoms, your doctor may suggest you see your eye specialist for an exam every year or two after age 40. If you develop pain, severe redness, or light sensitivity, consult an ophthalmologist.
Originally published in May 2016 and updated.


 Bone Spurs on the Spine
Bone Spurs on the Spine  Knee Injections for Osteoarthritis Pain Relief
Knee Injections for Osteoarthritis Pain Relief  What Is a Slipped Rib?
What Is a Slipped Rib? 
Bone pain can prompt such procedures as x-rays, MRIs, or ultrasound tests in search of a diagnosis.
© Tyler Olson | Dreamstime.com