Lumbar Pain: Causes and Treatments for a Common Affliction
Lumbar pain or low back pain is alarmingly common—and a major cause of lost productivity and activity restriction. So what are the causes of lumbar pain, and what should you do if you're suffering?
Low back pain is extremely common and affects most people at some point in their lifetime. Estimates show that up to 36 percent of us will suffer from a new or recurrent episode of low back pain in a given year. Much of it originates in the lumbar area. If you’ve experienced lumbar pain, you know it can have a significant effect on quality of life—the ability to work and participate in family and community routines.
Many environmental and personal factors influence your risk for developing lumbar pain. The incidence increases with age up to the age of 60, after which it declines.
Risk Factors for Lumbar Pain
Manual work, especially with vibrating tools, increases the risk of lumbar pain, but office workers are not immune, because long periods of inactivity are bad for the back. Lumbar pain is also associated with pregnancy, obesity, poor physical fitness, high levels of stress, anxiety, and depression.
Children can also suffer from lumbar pain due to “backpack overload.” The American Academy of Orthopaedic Surgeons suggests that backpacks should weigh no more than 15 to 20 percent of a child’s body weight.
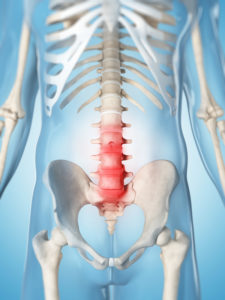
The lumbar spine, which sits below the thoracic spine (chest) and above the sacrum, consists of five movable vertebrae (L1 through L5).
Anatomy of the Lumbar Spine
The lumbar spine lies below the thoracic spine (chest) and above the sacrum. It consists of five movable vertebrae numbered L1 through L5, linked by a complex array of discs, joint capsules, ligaments/tendons, and large muscles. It also has a complicated, sensitive nerve and blood supply.
This region of the back is incredibly strong, yet highly flexible, allowing you to bend forwards, backwards, and sideways and to rotate your torso while at the same time protecting the delicate spinal cord running through the center of the vertebrae.
Causes and Symptoms of Lumbar Pain
Lumbar pain typically results from these causes:

More than a third of the adult population will experience new or recurrent low back pain in a given year, and it often originates in the lumbar area. Lumbar pain owing to strains or sprains often resolves itself with thermal therapy, pain relief, and rest.
- Sprains and strains. These affect the soft tissues of the lumbar region. They usually present with tightness, stiffness, muscle spasm, and pain upon moving the torso.
- Disc problems. Wear and tear to the soft cushion between the lumbar bones causes compression on the lumbar nerves, known as sciatica. Pain varies in intensity and may be accompanied by shooting pains in the leg and sometimes numbness or weakness in the buttocks or legs. Pain often worsens with sneezing.
- Spinal stenosis. Narrowing of the central channel within the lumbar bones (carries the spinal cord), leads to compression of the spinal cord and lumbar nerves. Pain is usually felt in the lower back when standing up, bending backwards, or walking, and it settles at rest. Pain may also be felt in the buttocks or legs.
- Osteoarthritis. This is more common in the limb joints but can also occur in the spine. Pain is usually intermittent.
- Ankylosing spondylitis. This is an inflammatory condition affecting the lumbar spine, beginning before the age of 40. Back pain and stiffness is progressive and over time spine movement becomes limited.
- Spondylolisthesis. Here an anatomical defect or injury allows one of the vertebra to slip forward.
- Referred pain from the abdomen. Sometimes inflammation, injury, or infection in the abdominal organs, including the bowels, reproductive system, and urinary tract, causes back pain.
Serious Causes of Lumbar Pain
- Cauda equina syndrome. This occurs when there is a severe disc herniation that presses on multiple nerves at once.
- Vertebral fracture. This is hard to diagnose, pain tends to be severe and localized but may also radiate to other areas. Pain increases with movement.
- Infection. This is rare but serious. Back pain is severe and accompanied by local redness or generalized fever.
- Spinal tumors. Back pain worsens over time and may be accompanied by numbness, pins and needles and weakness.
LUMBAR PAIN RED FLAGS
Call your doctor if you develop:
- Sudden onset of severe lumbar pain.
- Intense back pain lasts several days and prevents you from doing everyday tasks.
- Lumbar pain with:
- Fever and/or sweating.
- Sudden or increasing pain in legs.
- Bowel or bladder incontinence.
- Impotence.
- Numbness in anal area or groin.
Investigations and Tests for Lumbar Pain
If you are uncertain about the cause of your lumbar pain, your primary care physician is the place to start. He or she will take a full medical history and ask you about the onset and timeline of the pain and other symptoms. Clinical examination will include your back, pelvic area and legs, nerves, and blood supply.
If warranted, your physician may then go on to order further investigations, including:
- Blood tests to look for general markers of illness and inflammation.
- Specific tests such as HLA-B27 gene for ankylosing spondylitis and rheumatoid factor for rheumatoid arthritis.
- X-rays to look for bone abnormalities and significant anatomical changes. This is the first-line investigation in most cases of persistent or significant lumbar pain.
- Computed tomography (CT scan) to look for arthritis and spinal stenosis.
- Magnetic resonance imaging (MRI), the test of choice for suspected soft tissue problems like disc prolapse and tumors and to look at the nerves.
- Myelography to look for positioning of the nerves. Myelography involves fluoroscopic injection into the spinal canal, which houses the spinal cord.
- Bone scans are sometimes requested if a tumor or severe osteoporosis is suspected.
- Electromyography and nerve conduction tests can be useful if there is suspected nerve damage.
Your clinician may recommend that you see a specialist for further investigations. Possible options: a neurologist, neurosurgeon, orthopedist, or rheumatologist. Alternatively, your clinician may recommend that you see a physical therapist, chiropractor, osteopath, or physiatrist (rehabilitation specialist) for treatment.
Lumbar Pain Treatment: Home Remedies
There is an expression in medicine that goes, “Common things are common”—and this is certainly the case with lumbar pain. Most lumbar pain is caused by strains and sprains that will settle in a few days with simple remedies.
If your pain is mild to moderate and you do not have any of the red flag symptoms, the National Institute of Neurological Disorders and Stroke recommends the following:
- Thermal therapy. Applying heat and/or cold to the painful area has long been recommended for back pain. It can help relax tense muscles, increase blood flow and numb the pain (pain gating), but does not cure the underlying problem.
- Pain relief. Over-the-counter pain relief with non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen help reduce pain and calm inflammation. If you cannot take NSAIDs, try acetaminophen. If needed, your doctor may prescribe a short course of stronger pain relievers.
- Rest. In the short-term bed rest can help ease the pain but is not recommended for more than a day or so. The aim is to find a position that reduces the pain. If the pain is so bad that you can’t get out of bed, it’s time to see a doctor.
- Gentle movement. The goal is to “start low and go slow”: Be cautious, start with easy movements, and build gradually if the movements don’t exacerbate the pain. Stay clear of high-impact or twisting exercises when you have acute lumbar pain such as running, basketball, rowing, and even golf.
- Strengthen your core. Lack of core strength—weak muscles in the lower abdomen and pelvis—is a common cause of strains, sprains, and disc problems. Core strengthening exercises can be very helpful, but not in the acute stage of lumbar pain.
Exercises should be done with great care; if you do them wrong, you can do more harm than good. If you are unsure, a physical therapist or rehab specialist (physiatrist) will be able to guide you.
Therapy for Lumbar Pain
Various types of therapy also can help lumbar pain:
- Physical therapy. For starters, physical therapy can help strengthen the core, improve mobility and flexibility, and promote better posture.
- Massage, acupuncture, or spinal manipulation. Chiropractors, acupuncturists, and massage therapists specialize in these approaches for strains, sprains, and minor misalignments. The American Academy of Family Physicians reports that the evidence for the effectiveness of these modalities is “low quality,” but many people swear by them. Get recommendations from local friends for a good therapist. If you don’t see considerable improvement within six sessions of any approach, then it is unlikely to be of further benefit. (These approaches are not recommended for people with osteoporosis, nerve involvement, or inflammatory conditions such as rheumatoid arthritis.)
- Other treatments. Your doctor may also recommend a variety of other treatments, depending on your diagnosis including: Biofeedback, nerve block therapies, epidural steroid injections, and transcutaneous electrical nerve stimulation (TENS).
Another Option: Surgery
Surgery may be considered when other treatments fail or if there’s a serious underlying cause (such as spinal stenosis).
A variety of surgical techniques are available, from vertebroplasty for compression fractures due to osteoporosis, spinal laminectomy for spinal stenosis, and discectomy for severe herniation of a disc. Your surgeon will advise you on the best surgical procedure for your condition and general health.


 Vestibular Migraine Diet
Vestibular Migraine Diet  Bone Spurs on the Spine
Bone Spurs on the Spine  Knee Injections for Osteoarthritis Pain Relief
Knee Injections for Osteoarthritis Pain Relief 
The lumbar spine is strong and flexible but can become weakened by a wide variety of causes. Lumbar pain can arise from sprains and strains, disc problems, spinal stenosis, and osteoarthritis, among other factors.
ID 61376751 Juan Moyano | Dreamstime.com