Is Your Kidney Stone Pain a Single Episode… or Chronic?
Falling under the general heading of “plumbing,” your body’s waste filtration and elimination system toils silently—until something goes amiss. If your kidney stones are chronic, you and your physician need to formulate a plan of attack.
It started as a pain in the mid-back, disassociated from any kind of spinal or muscle soreness that sometimes accompanies strenuous activity. It was a dull ache, off to one side, and it persisted into a dark and rainy night…. I’d heard about kidney stones and thought I might be experiencing one. A friend described kidney stone pain as no less than breathtaking, driving him to his knees. And when I wound up in a fetal position on the floor, my faint suspicions grew firm.
A trip to the ER and an x-ray confirmed it—a kidney stone was just exiting my right kidney at the ureter, the tube that moves urine from the kidney to the bladder. A nurse said my urine sample looked “a little rich” with blood, and a physician said the best course would involve pain pills…and patience.
This too would pass, he said.
The pain pills helped, but a trip the next day to my exceptional urologist, Dr. Gerard Curtis in Sarasota, Fla., didn’t offer much comfort. His staff equipped me with a little screen to pee into in the hopes of catching the stone.
When I successfully captured the little devil the next day, the word “stone” failed to do justice. It looked like a meteorite—jagged, misshapen, ghastly. A real troublemaker.
But I was lucky. My bout with kidney stones appears to have been a singular event. A lot of people have chronic kidney stones, and relieving symptoms is a matter of working closely with your urologist to prevent them if you can, and to deal with them efficiently if you can’t.
Kidney Stone Pain: How It Starts
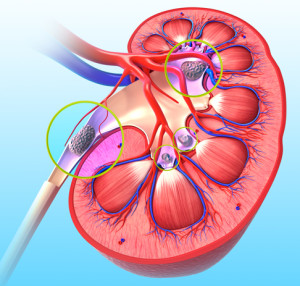
What causes kidney stones? They start with high levels of calcium, oxalate, and phosphorus in the urine before growing to sizes that are difficult to pass. [Photo: © Shubhangi Kene | Dreamstime.com]
According to the National Institute of Diabetes and Digestive and Kidney Diseases, kidney stones result when substances in the urine become highly concentrated.
Calcium stones, the most common type of kidney stone, come in two forms: calcium oxalate and calcium phosphate. Uric acid stones develop when urine is persistently acidic and can be caused by foods rich in purines found in animal protein, fish, and shellfish. A diet high in purines also factors in the development of gout.
Less common kidney stones are called struvite stones, often the result of a kidney infection or, rarer still, cysteine stones, which can result from a genetic disorder.
Kidney Stone Pain: Risk Factors and Treatment
Anyone can get a kidney stone, but men are more likely than women to develop the condition, and kidney stones are more common in non-Hispanic white people. Overweight and obese people are more likely to get kidney stones than people of normal weight.
A serious bout of kidney stones—especially if they happen periodically—can be treated medically or with surgery. But surgery is considered a last option. There are plenty of things you can do to deal with a stone, or prevent a stone from happening in the first place, especially if you are prone to producing them periodically. (See also our post “Natural Remedies for Kidney Stones.“)
According to Fredric Coe, MD, of the University of Chicago, no other condition lends itself so completely to the patient-physician partnership. Working with your doctor to monitor your condition, taking active steps, and feeding back information will greatly assist treatment and relieve kidney stone pain.
“At the end of it all, the science, the medical visits, the surgeries, what we really want is to prevent new stones,” according to Dr. Coe. “Modern surgery is a blessing for those with stones. But no surgery is far better than even the most skilled and effective surgery.”
Dr. Coe advocates a five-step approach to dealing with kidney stone pain and kidney stones:
- Know the stone crystals: Identifying the type of stone you are passing and capturing (remember that little screen) will lead to faster and more effective treatment. For instance, uric acid stones are easy to treat by adjusting urine pH levels. A cysteine stone is likely hereditary and requires special management. A struvite stone is likely the result of a kidney infection and may require surgery.
- Obtain proper blood and 24-hour urine measurements: Dr. Coe suggests your doctor will be able to interpret a standard 24-hour urine kidney stone risk panel to identify supersaturations that can develop into stones, along with urine chemistries that control those supersaturations. “These are the keys to prevention,” he says.
- Lower supersaturations for crystals in stones: Factors that raise supersaturations that lead to kidney stones include high urine calcium, high urine oxalate from diet, lower urine citrate and low urine pH (for uric acid stones) and high pH for calcium phosphate stones. Raising urine volume with fluid intake is critical in reducing supersaturations.
- Undergo more testing if stones continue: “Crystals follow physical laws and supersaturation is what drives them to form and grow,” according to Dr. Coe. “Continued stones with reduced supersaturations means either supersaturations need to be lower, or the 24-hour samples are not being taken on representative days.” Patient involvement is key to monitoring the condition.
- Annual follow-ups: Dr. Coe likes to use an aviation metaphor when advocating patient diligence to deal effectively with chronic kidney stones. “Lab measurements are the compass and altimeter,” he says. “Flying blind is silly.”
OUR BLOG LOG
Besides authoring informative, straightforward, easy-to-understand posts on a variety of medical issues, conditions, and treatments, our consumer health experts use a personal touch to help inform you via our series of UHN blogs.
- Aging & Independence: “What’s Ailing You? We’re All Ears” by Timothy Cole
- Bones & Joints: “Emergency! Coping with a Broken Ankle Overseas,” by Timothy Cole
- Cancer: “A Crusade Against Cancerous Moles,” by Jim Black
- Digestive: “Blood Tests, My Liver, and Me,” by Timothy Cole
- Eyes, Ears, Nose, & Throat: “Antibiotics Are Over-Prescribed,” by JoAnn Milivojevic
- Eyes, Ears, Nose, & Throat: “How to Get Through Allergy Season,” by Jay Roland
- Heart Health: “What’s the Right Blood Pressure for You?” by Jay Roland
- Nutrition: “What Is Nutrition?” by Dawn Bialy
- Pain: “How to Relieve Lower Back Pain,” by Kate Brophy
- Pain: “Is Your Kidney Stone Pain a Single Episode… or Chronic?” by Timothy Cole
To be a good kidney stone patient, according to Dr. Coe, requires preparation. Come to appointments with any stones you’ve collected. In addition, be sure to bring:
- All stone analyses
- Prior records
- Any imaging studies like CT scans or other radiographs
- Recent blood measurements
- Any 24-hour urine kidney stone tests to date
I haven’t had a recurrence of kidney stones in more than five years. But I have paid a little more attention to the BUN and creatinine levels on my recent blood test, both measures of kidney health. By consulting the American Association for Clinical Chemistry website, I learned that BUN stands for blood urea nitrogen. If BUN value in the blood increases, then the kidney is working less effectively and kidney (and possibly liver) damage may be in the cards.
Likewise, your creatinine level is also indicative of kidney health. Creatinine is a waste product produced by working muscles. Elevated creatinine levels indicate potential kidney failure.
Between my BUN, my creatinine, and my avoidance of kidney stones, I am feeling rather friendly toward my kidneys these days, which function benignly in the background, happily ignored. Like a lot of things in this carcass of mine, I didn’t really appreciate my kidneys’ value until one of them stopped working the way it was supposed to.
Originally published in August 2016 and updated.


 Vestibular Migraine Diet
Vestibular Migraine Diet  Bone Spurs on the Spine
Bone Spurs on the Spine  Knee Injections for Osteoarthritis Pain Relief
Knee Injections for Osteoarthritis Pain Relief 
It felt like a meteorite, our blogger writes, but his experience with a kidney stone pain began and ended with one episode.
Photo: Dreamstime.com