Chronic Obstructive Pulmonary Disease: Get COPD Diagnosed Early to Preserve Lung Function
Tell your doctor if you've been experiencing chronic cough and/or shortness of breath. It may be a sign of chronic obstructive pulmonary disease (COPD).
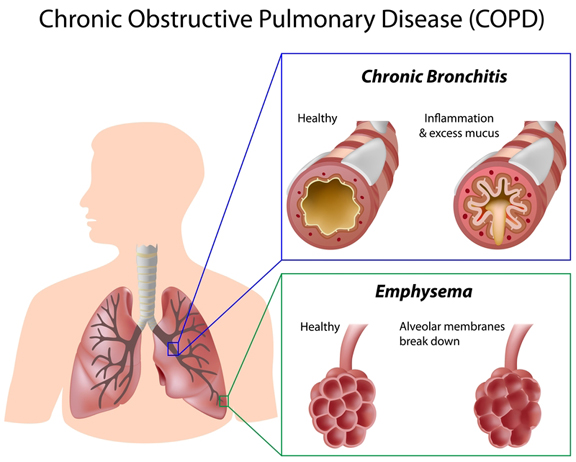
Chronic obstructive pulmonary disease (COPD) is a term for lung diseases that include emphysema and chronic bronchitis. Women are 37 percent more likely than men to have COPD, and it is the third leading cause of death in the U.S. COPD is undiagnosed in many patients who have it, but getting diagnosed and treated if you have COPD can help stop the condition from progressing.
“Medication can improve lung function and quality of life in patients with COPD, so it’s important for women with COPD symptoms, such as shortness of breath or a chronic cough, to report them to their doctors,” advises Kirana Gudi, MD, assistant professor of medicine at Weill Cornell Medicine.
Chronic Obstructive Pulmonary Disease Symptoms: Often Unreported
Common symptoms of COPD are dyspnea (shortness of breath), chronic cough, and sputum (mucous or phlegm) production. However, these symptoms are often overlooked or minimized.
“In the early stages of COPD, patients may only exhibit shortness of breath with exertion, such as when exercising or walking up stairs, and they may mistakenly attribute this to getting older or being ‘out of shape.’ When this is the case, patients frequently limit their activities to avoid these symptoms, and will therefore not report any shortness of breath when asked by their doctors. Additionally, some patients attribute their cough or phlegm to being simply a ‘smoker’s cough’ and not a pathological entity,” says Dr. Gudi.
The most significant risk factor for COPD is current or prior tobacco use, and patients who currently smoke often are reluctant to report symptoms. “Patients feel guilty talking about their symptoms with their doctors when they are actively smoking. This is unfortunate, because it prevents patients from being treated for their disease,” notes Dr. Gudi.
COPD Consequences
For some COPD patients, a chronic cough and shortness of breath may be considered bothersome, but not a cause for serious concern. However, an exacerbation (worsening) of symptoms can result in a feeling of choking or being unable to get enough oxygen, and it can be fatal, especially if medical treatment isn’t immediately available.
“Sometimes, a COPD exacerbation occurs due to an additional ‘trigger,’ such as an infection or some other stress to the body,” explains Dr. Gudi.
During an exacerbation, patients may experience increased shortness of breath and/or the inability to catch their breath. If they have a chronic cough, it may become more frequent and more severe, and their sputum may increase in amount or change in color. Patients also report hearing themselves make wheezing or whistling noises when they breathe.
For severe exacerbations, some patients require brief treatment with oxygen, and sometimes they require hospitalization. The goal is to keep these exacerbations to a minimum and to prevent further lung damage.
A Simple Test
The most common test for chronic obstructive pulmonary disease (COPD) is lung spirometry, a test which typically will show airflow obstruction if COPD is present.
“Any former or current smoker should be asked about symptoms of COPD and screened with spirometry if they have symptoms,” says Dr. Gudi. If you are having symptoms, don’t wait until your next regularly scheduled checkup; call your doctor and make an appointment.
Chronic Obstructive Pulmonary Disease Treatment Options
The goals of treatment for COPD are to control symptoms, improve function, and decrease exacerbations. “The ‘gold standard’ medications for patients with COPD are inhaled bronchodilators,” says Dr. Gudi. “Bronchodilators work by opening up the airways. They have been shown to decrease exacerbation rates, improve lung function, reduce symptoms, and improve quality of life in patients with COPD.”
Bronchodilators may be short-acting or long-acting. Dr. Gudi notes that there are now inhalers that combine different classes of long-acting bronchodilators for patients with more severe disease. Sometimes, bronchodilators are given in combination with inhaled glucocorticoids (steroids).
“These medications help to decrease the inflammation within the airways, and this has been shown to decrease exacerbations. However, because inhaled steroids do not improve lung function and they can predispose certain susceptible individuals to pneumonia, they should not be the only treatment for patients with COPD,” cautions Dr. Gudi.
Medications that treat COPD include:
Short-Acting Bronchodilators
- Albuterol (Vospire)
- Levalbuterol (Xopenex)
- Ipratropium (Atrovent)
Long-Acting Bronchodilators
- Tiotropium (Spiriva)
- Umeclidinium (Incruse Ellipta)
- Salmeterol (Serevent)
- Formoterol (Foradil, Perforomist)
- Tiotropium and olodaterol (Stiolto)
- Umeclidinium and vilanterol (Anoro Ellipta)
Inhaled Glucocorticoids
- Fluticasone (Flovent)
- Budesonide (Pulmicort)
COPD Lifestyle Strategies
Several non-drug interventions can help manage COPD. “For patients who currently smoke, smoking cessation is first and foremost—it decreases the rate of decline in lung function,” says Dr. Gudi. If you smoke, talk to your doctor about treatment options for smoking cessation and/or use free resources online, such as smokefree.gov, to help you quit.
Dr. Gudi notes that pulmonary rehabilitation programs, which include exercise, education, and support, can be critical in restoring exercise capacity, decreasing shortness of breath, and improving quality of life. Your doctor can refer you to a pulmonary rehab program if you have been diagnosed with COPD.
“Oxygen therapy can improve survival and quality of life in some patients with advanced COPD,” adds Dr. Gudi. “Finally, there are surgical techniques, including lung resection and transplantation, that can be effective in select patients with COPD.”
For further reading, see these University Health News posts:


 What is a Pulse Oximeter?
What is a Pulse Oximeter?  Lung Detox or Lung Cleanse: Can You Clean Out Your Lungs Naturally?
Lung Detox or Lung Cleanse: Can You Clean Out Your Lungs Naturally?  Are There House Plants That Clean the Air?
Are There House Plants That Clean the Air? 
"Medication can improve lung function and quality of life in patients with COPD," says Kirana Gudi, MD, assistant professor of medicine at Weill Cornell Medicine, "so it’s important for women with COPD symptoms, such as shortness of breath or a chronic cough, to report them to their doctors."
© Designer491 | Dreamstime.com