The Pacemaker: Our Primer Explains How It Keeps Your Heart’s Rhythm In Step
A pacemaker can be lifesaving if your heart is off-rhythm or weakened by heart disease. Here's how pacemakers work.
Do you have a pacemaker? If so, you’re benefiting from one of the most important developments in the history of medical technology. When the heart’s natural timing circuits go on the fritz, and if medication falls short, pacemakers can come to the rescue. Heart conditions that used to be fatal can now be essentially cured by implanting a small device in the chest during an outpatient surgery.
The Heart’s Natural Pacemaker
The heart is a fist-sized pump made out of muscle. To pump blood efficiently, two upper chambers (atria) and two larger, lower chambers (the ventricles) have to contract in the right order and at the proper rate.
The heart has its own internal pacemaker. It’s called the sinus node, and it lies near the top of the heart. Cells in the sinus node generate electrical impulses that travel downward along specialized cells in the heart.
The impulses help maintain the proper timing or “pacing” of the heart to pump blood through the heart’s four chambers. Normal pacing includes both the right heart rate (how fast the heart beats) and the proper rhythm.
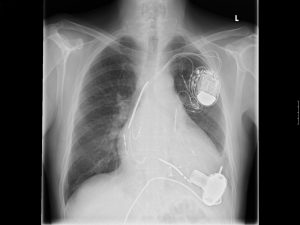
Pacemaker insertion involves a roughly 2-inch incision in the upper-left chest area, under the shoulder. (Photo: Photo 47955864 © Jfspic – Dreamstime.com)
How a Pacemaker Is Implanted
Pacemakers are implanted just below the skin surface in the left upper chest. The typical incision required is about 2 inches long. You’ll normally be awake for the implant, with local anesthesia to numb the area where the pacemakers will be inserted. You’ll take a sedative to relax you during the procedure, though you will remain otherwise conscious.
If you experience complications after the implant procedure, it usually will be one of these:
- Swelling, bleeding, bruising, or infection around the implant
- Damage to blood vessels or nerves
- Collapsed lung
- Adverse reaction to medication used during the procedure
What Does a Pacemaker Do?
Pacemakers do not replace the heart’s natural pacing system. They just help to keep the heart’s natural rhythms on track if they’re not working properly.
Electrical impulses from the pacemaker make sure the different chambers of the heart contract (squeeze inward) in a coordinated way. This keeps blood flowing to the rest of the body despite abnormalities in the heart’s natural rhythms.
How Does a Pacemaker Work?
A typical pacemaker is roughly the width of a half-dollar and several times thicker. The device includes a tiny pulse generator, a battery, wiring, and a computer.
Insulated wires, called leads, are run from the pacemaker, through veins, and into the heart. Pacemakers can have one, two, or three leads, depending on the type of arrhythmia and the therapy needed. Most pacemakers implanted today have two leads—one to the right atrium and the other to the right ventricle.
The pacemaker’s circuits monitor your natural cardiac rhythm and deliver tiny jolts to where they are needed to make the heart operate properly. Most pacemakers also can sense your breathing and physical motion, allowing them to tune your heart rate to the body’s needs.
The pacemaker’s battery is internal, so the entire device has to be swapped out when the battery runs out. Pacemaker batteries can last five to 15 years, though the average is around six to seven years.
Who Needs a Pacemaker?
Pacemakers help people with abnormal heart rhythms (arrhythmias) that can’t be treated adequately with antiarrhythmic drugs. Arrhythmias take many forms. The three general types are:
- Premature, or extra, heartbeats, also called palpitations. These can occur in the atria or the ventricles and are usually harmless, though they can be unpleasant.
- Fast heartbeat, or tachycardia, in which the resting heart rate is faster than 100 beats per minute. One of the most well known is atrial fibrillation, which can cause blood clots to form in the atria. Other, more dangerous, forms of fast heart beat are ventricular tachycardia and ventricular flutter. These can cause sudden cardiac death.
- Slow heartbeat, or bradycardia, in which the resting heart rate is less than 60 beats per minute. A condition called sick sinus syndrome can cause slow heartbeat (with symptoms), which is the most common reason people get pacemakers. (See also our post Is a Low Heart Rate Dangerous?)
Arrhythmias cause some distinctive types of symptoms. The most common that people report include:
- Weakness
- Fatigue
- Lightheadedness
- Dizziness
- Temporary loss of consciousness (syncope)
Pacemakers and Heart Disease
People sometimes develop slow heartbeats after a heart attack, which temporarily interrupts the supply of oxygen-rich blood to heart muscle. Bad reactions to medications and physical trauma to the heart (as during a car accident) also can cause bradycardia. In such cases, a pacemaker might be installed temporarily until the function of the heart returns to normal.
Pacemakers also are used to treat heart failure. Heart failure is when the heart is unable to pump enough blood to meet the body’s needs. In such cases, a special type of pacemaker can provide cardiac resynchronization therapy (CRT). This is for people with heart failure experiencing moderate to severe symptoms, and whose left and right heart chambers do not beat in unison.
In CRT, a special pacemaker pacemaker helps the ventricles on both sides of the heart to work together. The device that does this is called a biventricular pacemaker. One lead goes to the right atrium and the other two go to the right and left ventricles.
Some people with heart failure are at significant risk of sudden cardiac death caused by fast or uneven beating in the heart’s main pumping chambers. In such cases, a person can get an enhanced pacemaker called an implantable cardioverter-defibrillator, or ICD.
The ICD provides pacing to maintain optimal cardiac rhythms and also can shock the heart back to normal rhythm if it develops dangerous ventricular rhythms. The device is larger than a normal pacemaker—about the size of a cell phone. It is implanted either under your collarbone or in the abdomen.
You have probably seen the full-size equivalent of an ICD hanging in boxes on the walls of public buildings. The boxy device is an automated external defibrillator, or AED. These can be used to save a person’s life if they go into cardiac arrest from ventricular arrhythmia.
Living with a Pacemaker
Pacemakers are reliable and safe but you need to make certain adaptations once you have one:
- After the pacemaker is installed and programmed in the hospital, you’ll need to return for a follow-up visit so your doctor can make sure the device is functioning correctly.
- Longer term, you will receive equipment to take home that can wirelessly connect to the pacemaker, collect information, and send it to your cardiologist.
- A pacemaker can trip metal detectors. When passing through security checkpoints in airports and other public spaces, tell the security screener you have a pacemakers. The screener should not pass a handheld metal detector “wand” close to the pacemaker, since it has a magnet inside. Full-body scanner should not cause any problems with your device, but check with your doctor.
- Inform any doctor you see that you have a pacemaker, if they don’t already know.
- You will need to avoid having an MRI or take special precautions. Medical staff are trained to handle this risk.
- Radiation therapy for cancer can damage a pacemaker, so you will need to take special precautions. Again, medical staff are trained to handle this issue.
- A large variety of electric and electronic devices can interfere with a pacemaker. Make sure your healthcare providers have educated you fully about this. Mainly, you need to avoid or stay a safe distance from electrical equipment that can send out signals that could interfere with the pacemaker. That includes cell phones or magnets (if held too close to the pacemaker), electric blankets, high-voltage transformers, welding equipment, electrical generators, and some electric tools.
- If you have an ICD and it trips, it can feel like a kick in the chest. This can be alarming and upsetting, but the alternative might have been sudden death.


 News Briefs February 2024
News Briefs February 2024  Savor the Sweet Potato
Savor the Sweet Potato  What Are the Dangers of Erythritol?
What Are the Dangers of Erythritol? 
A pacemaker device features a tiny pulse generator along with a battery, wiring, and a computer.
Photo 50726962 © Mohammed Anwarul Kabir Choudhury - Dreamstime.com