Epididymitis Treatment: With Prompt Attention, You Can Avoid Complications
If you experience testicle swelling, pain, or other signs of scrotal infections, it may be a condition known as epididymitis. Treatment can clear it up.
An infection can occur almost anywhere in the genitourinary system. In fact, urinary tract infections are so common, they’ve been branded with a widely used abbreviation: UTI. Scrotal infections such as epididymitis aren’t as common as UTIs and haven’t earned a convenient abbreviation, but they can be extremely painful and debilitating. They also can lead to lingering complications if left unchecked. That’s why it’s important to recognize the warning signs and to begin prompt epididymitis treatment.
Risk Factors | Symptoms | Treatment
What Is Epididymitis?
On the backside of each testicle sits the epididymis, a coiled duct that serves as a reservoir for sperm while they mature and that also carries sperm from the testicle to the vas deferens, the conduits that allow sperm to be released through ejaculation. Epididymitis occurs when the epididymis becomes inflamed, usually as a result of a bacterial or viral infection. Infections also are the primary cause of orchitis, inflammation of one or both testicles.
Acute epididymitis has symptoms lasting less than six weeks, while chronic epididymitis symptoms like six weeks or longer with a more gradual onset. Epididymitis also can spread to the testicle, resulting in a condition known as epididymo-orchitis.
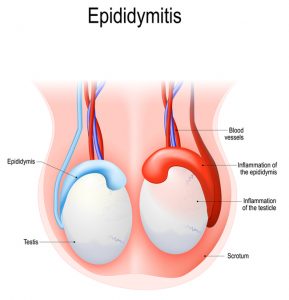
Epididymitis is an inflammation of the epididymis of the testicle.
Who’s at Risk for Epididymitis?
Epididymitis can occur in men of all ages. Among younger men, sexually transmitted infections, namely chlamydia and gonorrhea, are to blame in most cases. Among men over age 35, epididymitis caused by sexually transmitted infection is uncommon, according to the Centers for Disease Control and Prevention (CDC). In these men, epididymitis may occur when bacteria from a urinary tract infection or prostatitis (prostate infection) migrate to the epididymis.
Other potential contributors to epididymitis in these men include infections resulting from urinary tract surgery, insertion of a catheter or scope into the urethra, and obstructive urinary disease caused by an anatomical abnormality in the urinary tract or benign prostate enlargement (BPH). Injury to the scrotum and use of the drug amiodarone (Pacerone), used to treat irregular heart rhythms, can trigger epididymitis. In rare cases, tuberculosis infection can cause epididymitis.
Epididymitis Symptoms
Men with epididymitis or epididymo-orchitis may experience one or more of the following symptoms:
- Pain, tenderness, heaviness, or pressure in and around the affected testicle
- A swollen or inflamed scrotum
- Testicle swelling/lump on the testicle
- Lower abdominal and pelvic/groin pain
- Urinary symptoms, such as painful urination or increased urinary frequency
- Pain during intercourse or ejaculation
- Discharge from the penis
- Blood in the semen (hematospermia)
- Chills and fever
See your doctor if you experience these symptoms. Also, keep in mind that sudden testicle swelling or pain may signal testicular torsion, a twisted testicle that requires emergency treatment.
Epididymitis Treatment
Epididymitis left untreated can become chronic. Broad-spectrum antibiotics are the cornerstone of bacterial epididymitis treatment. Finish the entire antibiotic prescription, even if your symptoms resolve sooner, and follow up with your doctor to make sure the infection has cleared. If chlamydia or gonorrhea have caused your infection, your sexual partner also should be tested and treated.
In addition to antibiotics, epididymitis treatment may entail the use of analgesic medications to ease pain, as well as ice packs, elevation of the scrotum, and bed rest to relieve discomfort. Less commonly, surgery may be necessary to remove all or part of the epididymis, to correct any anatomical abnormalities that are contributing to epididymitis, and to drain an abscess caused by the infection.
In most cases, epididymitis and orchitis cause no further complications, but some patients—such as those who can’t take oral medications, men who don’t improve within a few days with outpatient treatment, and men who have significant symptoms and compromised immune systems—may need to be hospitalized.
Originally published in 2017, this post is regularly updated.



 Can Prostate Supplements Reduce Your Risk of Prostate Cancer?
Can Prostate Supplements Reduce Your Risk of Prostate Cancer?  What Is Robotic Prostatectomy & The Advantages of Robotic Surgery
What Is Robotic Prostatectomy & The Advantages of Robotic Surgery  What Can Skew a PSA Test? These 10 Factors Can Affect Your Numbers
What Can Skew a PSA Test? These 10 Factors Can Affect Your Numbers 
Epididymitis treatment begins with a doctor's evaluation.
© Syda Productions | Dreamstime.com