Prostate Gland Cancer: Testing and Diagnosis
How do doctors determine you have it? Which tests are most reliable?
If your doctor has determined that you’re experiencing prostate cancer symptoms and that your otherwise normal PSA levels are elevated, he likely will order a biopsy of tissue from the prostate gland.
Your doctor may elect to biopsy your prostate based on whether or not you have possible symptoms of prostate cancer, on your PSA levels, and/or on your digital rectal exam (DRE) findings.
There are differing opinions among professional medical organizations about whether performing a biopsy based on abnormal PSA results alone is appropriate. A number of other tests (e.g., PCA3 and PSA velocity) have been developed as screening tools in an effort to either avoid unnecessary biopsy or improve prostate gland cancer detection. Most experts agree, however, that there isn’t enough evidence yet to make them part of a routine screening process. You and your healthcare provider should discuss these options prior to a biopsy.
If prostate cancer is suspected, your doctor will perform a biopsy guided by transrectal ultrasound. A small ultrasound probe is inserted into the rectum to guide the biopsy needle to the biopsy locations. The needle is inserted through the wall of the rectum into the prostate gland to retrieve small pieces of tissue. Typically, at least 12 samples of tissue are taken from different areas of the prostate. This can be done on an outpatient basis and is usually a brief procedure.
The tissue samples are sent to a pathology lab for examination. If cancer cells are evident, they typically are graded using a system called the Gleason score, an indicator of how likely the cancer is to spread. Tissue from two different parts of the prostate gland are examined and given a score from 1 to 5; the numbers from each part are then added together to create the Gleason score. A lower score suggests a lower likelihood of spreading, while a higher score suggests a greater chance.
Once a diagnosis of prostate cancer has been made, additional tests will be performed to determine whether or not the cancer has spread beyond the prostate. These test results, along with the Gleason score, will be used to assign the disease a prostate cancer stage. The system most often used is the American Joint Committee on Cancer “TNM” system, which provides a Roman numeral staging score from I-IV based on the size of the primary Tumor, whether or not there is lymph Node involvement, whether the tumor has Metastasized, the PSA level at diagnosis, and the Gleason score.
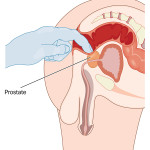
First line of defense in detecting prostate cancer is the digital rectal exam (DRE), plus a measurement for prostate specific antigen (PSA) in the blood. These steps are controversial, however, because some contend PSA has led to over-diagnosis and debilitating over treatment for cancers that aren’t lethal.
The more advanced the cancer, the higher the TNM stage number. For example, in stage I prostate cancer, the cancer has not spread beyond the prostate itself while in stage IV prostate cancer, the cancer has spread beyond the prostate, either to nearby organs and/or lymph nodes or to more distant sites in the body.
Tests performed to help stage the cancer may include:
- Computed Tomography (CT): CT scans are used to look for evidence of metastasis, particularly to lymph nodes.
- Magnetic Resonance Imaging (MRI): MRI is also used to look for evidence of metastasis.
- Bone Scan: Since bone is one of the most common places for prostate cancer to metastasize, bone scans are often used to look for disease spread.
- Positron Emission Tomography (PET): PET scans can also be used to look for evidence of metastasis. They are particularly helpful in looking for evidence of disease recurrence in men who have been previously treated for prostate cancer.
- Lymph Node Biopsy: Knowing whether or not your prostate cancer has spread to lymph nodes is an important part of determining what treatment regimen you should receive. Imaging tests such as CT scans can help provide information as to whether or not the lymph nodes are involved, but biopsying lymph nodes is the only way to definitively make this determination. If your doctor doesn’t anticipate surgery as a part of the treatment regimen, he may opt to biopsy your lymph nodes laparoscopically. In other situations, your surgeon may biopsy your lymph nodes during an operation to remove your prostate gland.


 Can Prostate Supplements Reduce Your Risk of Prostate Cancer?
Can Prostate Supplements Reduce Your Risk of Prostate Cancer?  What Is Robotic Prostatectomy & The Advantages of Robotic Surgery
What Is Robotic Prostatectomy & The Advantages of Robotic Surgery  What Can Skew a PSA Test? These 10 Factors Can Affect Your Numbers
What Can Skew a PSA Test? These 10 Factors Can Affect Your Numbers 
Cancer in the prostate gland, which sits under the bladder and emits fluid to aid in reproduction. It also encases the ureter descending from the bladder, so complications involving the prostate necessarily involve urination.