What Causes Cholesterol Abnormalities?
Some factors that could raise your risk of high cholesterol are under your control, while other factors aren't.
A number of factors—some preventable, others not—can cause abnormal cholesterol levels, or dyslipidemia, in the blood. Here are the factors that you can control:
A Poor Diet
Diets high in saturated fat and trans fat are linked to higher LDL cholesterol levels. Saturated fats are found in animal products, especially fatty red meat (beef and pork) and processed meats (sausage, bacon, salami), as well as full-fat dairy products.
Trans fats are found in partially hydrogenated oils (PHOs) produced by food manufacturers. Like saturated fats, trans fats can raise LDL cholesterol levels, but they also trigger reductions in HDL cholesterol.
PHOs are now scarce since the FDA ordered PHOs to be removed from food products by 2018 (although this deadline was extended to 2020 for some)—but it’s still wise to double-check ingredients lists for PHOs.
Physical Inactivity
A sedentary lifestyle can cause a decline in HDL, which leaves fewer of these LDL scavengers to remove the “bad” cholesterol from your bloodstream and arteries.
Conversely, research suggests that staying (or becoming) physically active can increase HDL levels and also increase the size of LDL particles, making them less dangerous.
 Obesity
Obesity
If you’re overweight or obese, you’re more likely to have higher LDL and triglyceride levels and lower HDL levels. Losing weight may help restore a better cholesterol balance.
Smoking
Like a sedentary lifestyle, tobacco smoking has been shown to reduce healthful HDL cholesterol. Research suggests that quitting smoking can help improve your HDL count.
Medical Conditions
Several medical conditions can adversely affect your lipid profile:
- Diabetes. The high blood sugar of diabetes can contribute to elevations in LDL cholesterol and triglycerides and cause declines in HDL cholesterol. This condition is known as diabetic dyslipidemia. Research suggests that prediabetes, or insulin resistance—elevated blood-sugar levels that may precede type 2 diabetes—also is associated with diabetic dyslipidemia and cardiovascular disease. So, preventing type 2 diabetes by maintaining a healthy weight and adhering to a healthy diet and exercise regimen can have positive effects on your cholesterol.
- Sleep disorders. Some evidence suggests an association between failing to get enough sleep and a greater risk of atherosclerotic cardiovascular disease, including increases in blood pressure, cholesterol, and triglyceride levels. One study found that prolonged sleep loss was associated with alterations in genes that help regulate cholesterol transport and reduce levels of HDL cholesterol. More recent research suggests that obstructive sleep apnea, a common disorder characterized by repeated interruptions in breathing during sleep, may be linked to poorer lipid profiles (see “Sleep Apnea Linked to Unhealthy Lipid Patterns”).
- Thyroid dysfunction. The thyroid gland is important for cholesterol regulation. Hypothyroidism, or underactive thyroid, can cause increases in triglycerides, LDL, and total cholesterol. Some studies suggest that even a mild, asymptomatic form of the disease, known as subclinical hypothyroidism, may cause these elevations, but to a lesser extent. Correcting an underactive thyroid may help improve your lipid levels.
- Kidney disease. Elevated lipid levels often accompany chronic kidney disease, and research suggests that high cholesterol and triglycerides may be risk factors for kidney disease progression.
- Polycystic ovary syndrome. Women with this condition, caused by an imbalance of reproductive hormones, may have high LDL and low HDL levels, and are at increased risk of atherosclerosis.
- Pregnancy. Lipid alterations, such as increases in triglycerides and total cholesterol, can occur during pregnancy.
Medications
A number of prescription medications can affect cholesterol levels. Examples include:
- Blood pressure medicines. Thiazide diuretics, such as hydrochlorothiazide (Microzide), may cause temporary increases in LDL cholesterol and triglycerides. Use of older beta-blocker medications, such as atenolol (Tenormin), metoprolol (Lopressor, Toprol), and propranolol (Inderal), has been associated with slight increases in triglycerides and slight reductions in HDL cholesterol.
- Amiodarone. This drug, marketed as Cordarone and Pacerone, is used to treat irregular heart rhythms. The medication has been linked with higher cholesterol and triglyceride levels.
- Antipsychotic drugs. Several medications used to treat schizophrenia and other psychotic conditions are associated with increases in total cholesterol and triglycerides. Examples of these drugs include chlorpromazine (Thorazine), haloperidol (Haldol), loxapine (Loxitane), aripiprazole (Abilify), olanzapine (Zyprexa), and risperidone (Risperdal), among others.
- Corticosteroids. These potent anti-inflammatory drugs used to treat autoimmune conditions such as rheumatoid arthritis and lupus have been tied to increases in LDL cholesterol and triglycerides. Members of this drug class include dexamethasone, prednisone, and prednisolone.
- Antidepressants. Certain medications used to treat depression, such as desvenlafaxine (Pristiq) and venlafaxine (Effexor), may be associated with increases in LDL cholesterol and triglycerides.
These medications may potentially affect your lipid profile, but the extent to which they influence your cardiovascular risk remains unclear. Also, keep in mind that, in many cases, the benefits of these medications outweigh any potential risks posed by their lipid-altering effects.
 High Cholesterol Factors Beyond Your Control
High Cholesterol Factors Beyond Your Control
Age
Your cholesterol tends to rise as you get older, making advancing age a risk factor for high cholesterol.
Gender
Until menopause, women typically have lower LDL and total cholesterol levels than men do; however, following menopause, LDL cholesterol and triglycerides tend to increase, while HDL levels often decline or stay the same. LDL levels rise more quickly for women than for men, according to the Centers for Disease Control and Prevention (CDC), but men at any age usually have lower HDL levels compared with women.
Race
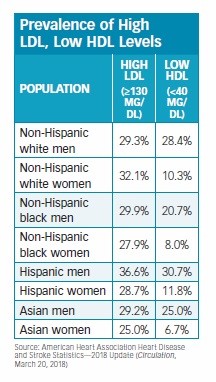
The American Heart Association’s 2018 heart disease and stroke statistics (suggest some variations in cholesterol levels among different races (see “Prevalence of High LDL, Low HDL Levels”).
Family History
Genetics plays a role in how much cholesterol your body produces. People with a family history of high cholesterol may be more likely to have high cholesterol themselves.
Research suggests that more than 800,000 American adults have a genetic condition known as familial hypercholesterolemia, which causes very high LDL cholesterol levels at a young age.
To learn more about the risk factors for cholesterol, purchase Managing Your Cholesterol at UniversityHealthNews.com.


 High Cholesterol Factors Beyond Your Control
High Cholesterol Factors Beyond Your Control News Briefs February 2024
News Briefs February 2024  Savor the Sweet Potato
Savor the Sweet Potato  What Are the Dangers of Erythritol?
What Are the Dangers of Erythritol? 
Several medical conditions can adversely affect your lipid profile.
ID 34298209 © Alexmillos | Dreamstime.com