Cluster Headache: How It Happens, How to Treat It
A cluster headache can manifest itself in bouts that hit at the same time of the day or night for weeks. Here's how to identify and treat cluster headaches.
A cluster headache is the “most severe form of primary headache,” as the U.S. National Library of Medicine tells us. When you get one, you’ll know it, because of the onset of sudden—and painful—headache clusters, usually at the same time of the day and night for several weeks. They typically affect one side of the head, often around or behind one eye. A migraine-like aura and nausea may precede a cluster headache.
Those who suffer from cluster headaches find they often last for about six to 12 weeks. In between attacks, there may be periods of remission that last weeks, months, or even years. In some people, cluster headaches can be chronic for up to a year or more with very few (and very brief) remissions. Men are more likely than women to suffer from the cluster headache phenomenon; the tendency also is more common in smokers. Alcohol (particularly red wine) may trigger an attack.
Cluster Headache Symptoms
As with migraine symptoms, cluster headache symptoms may be preceded by an aura, and tend to be focused on one side of the head. The pain of a cluster headache is sudden, piercing, and extremely severe; if you’re asleep when one strikes, it will likely awaken you. A cluster headache reaches peak strength within about 10 minutes and continues at that intensity for anywhere up to three hours.
You may feel restless during a cluster headache and notice that your heart is racing. Your blood pressure typically rises. The eye on the affected side of your head may swell, droop and tear, and you may notice increased sensitivity to light, sound, and odors.
Typical Cluster Headache Causes
It is thought that cluster headaches may be caused by a problem with the hypothalamus, a complex part of the brain that controls many of the body’s functions, including heart rate, blood pressure, temperature, appetite and sleep cycles. Imaging tests have revealed increased activity in the hypothalamus during a cluster headache. The trigeminal nerve, which transmits sensations from the brain to the face, also may be involved.
Other possible causes include nitroglycerin, which is used to treat heart disease. However, in general the triggers that may jumpstart other types of headache (for example, certain foods, stress, and/or hormonal changes) are not thought to influence cluster headaches.
FYI
WHICH HEADACHE?
Headaches can bring with them various symptoms and for different lengths of times. See these related University Health News articles:
- “Dehydration Headache? Know the Causes, Signs, and Symptoms”
- “Ice Pick Signs and Symptoms“
- “Exertion Headache?: Consider the Causes and Try These Treatments”
- “Tension Headache: What Causes It, How to Manage It”
- “What’s the Difference Between a Sinus Headache and a Migraine Headache?”
- “Headache Behind Eye? How to Spot Potential Brain Aneurysm Symptoms”
Cluster Headache Treatment and Prevention
The triptans that can be used to treat migraines also can be used to alleviate and prevent cluster headaches. Sumatriptin is particularly effective if delivered by injection, but isn’t suitable for people with high blood pressure or heart disease. Another triptan—zolmitriptan—is available in nasal spray and tablet form, and also works rapidly.
Calcium-channel blockers and anticonvulsants also may be used, as well as ergots, and corticosteroids. Other fast-acting treatment options include oxygen therapy, in which pure oxygen is breathed through a mask, reducing blood flow to the brain—some people report relief from a cluster headache within 15 minutes.
Rarely, in people for whom drugs provide no relief, a surgical procedure that uses heat to destroy certain facial nerves may be considered to treat cluster headaches. About 50 to 70 percent of people who undergo the procedure gain relief, but side effects (such as numbness, and muscle weakness in the jaw that can impede chewing) are common.
Researchers also are looking at the effectiveness of occipital nerve stimulation, in which an electrode is positioned under the skin at the base of the skull, near the occipital nerves, and connected by a wire to a small pacemaker-like device implanted elsewhere (typically under the collarbone). The device delivers mild electrical pulses to one or both nerves, and studies suggest it can improve cluster headaches for some people, although long-term data is lacking.
Deep brain stimulation (DBS), which is currently used to treat Parkinson’s disease, also is being investigated as a treatment for cluster headaches. The principle is similar to occipital nerve stimulation, but the electrode is implanted in the hypothalamus. Only a small number of people have been treated using DBS, but the results have been promising.
As far as alternative treatment is concerned, there is evidence that the hormone supplement melatonin may reduce cluster headache frequency—but let your doctor know if you try this.
Originally published in 2016 and regularly updated.


 Vestibular Migraine Diet
Vestibular Migraine Diet  Bone Spurs on the Spine
Bone Spurs on the Spine  Knee Injections for Osteoarthritis Pain Relief
Knee Injections for Osteoarthritis Pain Relief 
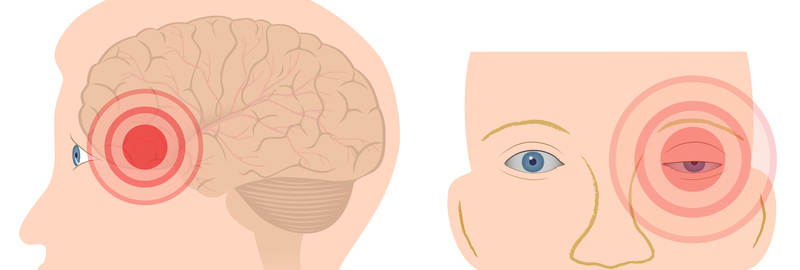
A cluster headache is characterized by a group of severe headaches that strike at once, usually on one side of the head, often behind or around an eye.
© Marijus Auruskevicius | Dreamstime.com