Are You Suffering from Jaw Pain?
Jaw pain might seem insignificant and turn out to be easily treatable and temporary, but for some, it may red-flag a more serious issue, from gum disease to heart attack.
Because your jaw is one of the joints you use most often, dealing with jaw pain can be difficult: It can affect your ability to talk, eat, and even concentrate. Often, jaw pain is related to problems with your teeth resulting from an oral health issue or from a habit like teeth grinding.
But jaw pain also can underpin other conditions, such as chronic headaches. And if you’re a woman with poor heart heath, jaw pain can even be a sign that you’re having a heart attack.
Below, we consider seven common causes of jaw pain, along with symptoms and treatment tips.
1. Gum disease and cavities
Gum disease, also referred to as periodontal disease, or gingivitis) involves infected gums that can become painful and lead to serious problems. The condition can lead to sore, swollen gums that bleed easily, as well as tooth loosening that can cause jaw pain.
You’re at greater risk for periodontal disease if you don’t have a regular, thorough oral care regimen, including annual checkups. Experts recommend brushing and flossing your teeth twice a day; using a water flosser, such as a WaterPik, also can help you avoid periodontal disease.
Other risk factors for gum disease include tobacco use (cigarettes and chewing tobacco), pregnancy, diabetes, and certain medications (including chemotherapy drugs and steroids). Gum disease also can develop if your teeth are crooked, which can make it difficult to brush properly.

An abscessed tooth is the culprit behind some cases of jaw pain. A dental exam and x-ray will reveal the answer.
2. Dental abscess
A dental abscess can develop due to gum disease and cavities, both of which can result in bacteria entering the soft pulp at the center of a tooth. If you have an abscess, you will likely suffer pain as well as swelling and redness in the area. You also may notice a bad taste in your mouth.
It’s important to consult a dentist if you develop an abscess. Untreated, it can result in serious jaw pain, particularly if it progresses to a jawbone infection.
3. Temporomandibular jaw (TMJ) disorder
If you have jaw pain and also find it difficult to open your mouth, you may be experiencing temporomandibular jaw disorder. The temporomandibular joints connect your lower jaw (mandible) to the temporal bone at each side of your face. The muscles and bones of the joints control the movements your jaw makes (back, forth, around, and sideways) as you chew, swallow, and speak
Problems such as arthritis, a misaligned jaw, teeth grinding, and stress can interfere with smooth movement, resulting in jaw pain that radiates to the front of your face as well as a stiffness in your jaws. You also may notice a clicking or popping sound when your jaw opens. In severe cases, your jaw may lock when opened wide (for example, during a yawn).
If you suffer from TMJ disorder, you may be able to ease the discomfort with painkillers (your doctor also may prescribe an antidepressant), and by applying heat packs to your jaw. Some people also gain relief by wearing a mouth guard over their teeth at night while they sleep. If these conservative measures don’t bring relief, ask your dentist about surgical options for treating TMJ disorder.
See also our posts TMJ Pain: 9 At-Home Treatments to Ease Jaw Discomfort and 7 Essential TMJ Exercises to Relieve Jaw Pain.
4. Teeth grinding
Habitual teeth grinding and/or jaw clenching is officially called bruxism. For many people, teeth grinding is a coping habit, a way of managing stress, and they don’t actually realize they’re doing it. It often occurs while they are asleep.
While the habit is mild in most people, more severe bruxism can result in jaw pain and also may underpin TMJ disorder. It also can damage the teeth; constant grinding can wear down the tough enamel that protects the sensitive inner layers of teeth. If you have jaw pain that radiates to your ears, constant headaches, and sensitive teeth that appear excessively worn, you may have bruxism.
As with TMJ disorder, your dentist may recommend you wear a mouth guard overnight to prevent teeth grinding. Another treatment: Stress management strategies such as meditation, which can help you relax and deal with mental challenges.
5. Trigeminal neuralgia
Sensation in your face is conducted by the trigeminal nerve, which also controls the movement of your muscles when you chew.
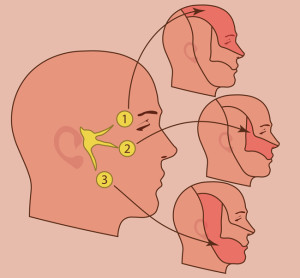
Trigeminal nerve inflammation can create jaw pain as well as pain in other parts of your head. [Photo: © Aleksei Fetisov | Dreamstime.com]
If you experience this intense, shooting pain in your face or jaw, consult your doctor. Anticonvulsant and antispasmodic medications can be prescribed to help control trigeminal neuralgia, and some people also report relief from Botox injections. Surgical options are available for severe cases.
6. Osteonecrosis of the jaw
The bisphosphonate medications many older adults take to help prevent the breakdown of bone that results in osteoporosis also can impact your jaw health. Bisphosphonates have been linked with a rare but serious side effect called osteonecrosis of the jaw (ONJ), which can result in infection and breakdown of the jawbone.
Concerns about ONJ are one reason why most people who take bisphosphonates are advised to stop the drugs after three to five years. However, in January 2016, an editorial from the International Osteoporosis Foundation (IOF) Working Group questioned this automatic break from bisphosphonates, saying that doctors needed to consider a patient’s risk for fractures before stopping the drugs.
The IOF also pointed out that the concept of a need for a break from bisphosphonates causes unnecessary worry in patients, given the rarity of ONJ compared with the fact that hip and spinal fractures are far more common and disabling in people with osteoporosis.
“There is much clinical confusion about best practice,” said lead author Stuart Silverman, MD, PhD, medical director of the Bone Health Center at Cedars-Sinai Medical Center. “We have little global consensus on how to identify which patients should have a drug holiday, and how to manage and monitor these patients. More research is needed so that we can provide physicians with clear recommendations.”
If you take bisphosphonates, be alert to the symptoms of osteonecrosis of the jaw. Among them: jaw pain, facial pain, swelling, numbness, and loose teeth.
7. Potential heart issue
Could your jaw pain signal a heart attack? Typical heart attack symptoms include a squeezing sensation in the chest, chest pain that radiates down one arm, and shortness of breath. But women especially are more likely to suffer atypical symptoms, including jaw pain as well as extreme fatigue, anxiety, and cold sweats.
If you have heart attack risk factors—among them high blood pressure, high cholesterol, diabetes, being overweight or obese, and smoking—get fully informed about heart attack risk factors, and report any, including unexplained jaw pain, to your doctor.
Originally published in 2016, this post is regularly updated.


 Vestibular Migraine Diet
Vestibular Migraine Diet  Bone Spurs on the Spine
Bone Spurs on the Spine  Knee Injections for Osteoarthritis Pain Relief
Knee Injections for Osteoarthritis Pain Relief 
Jaw pain can point to any of a number of causes, including the seven listed here.
© Sebastian Kaulitzki | Dreamstime.com